There is no part of urology that has made so much progress in the last 25 years as neuro-urology. Seminal developments have been made in the selective effectiveness of drugs influencing neurogenic lower urinary tract dysfunction but having limited side effects. Additional advances are also likely to be made in the methods of neuromodulation and tissue engineering. Neuro-Urology is predominantly influenced by our dynamic-functional understanding and the functionally oriented planning and implementation of treatment. The initial treatment options in many areas of neuro-urology are conservative, but, when possible, not irreversible. If these are ineffective or lead to late complications (e.g. by congenital paraplegia), there are a series of organ sparing or organ manipulating operations which can restore organ function. These make it possible to save renal function from continuing damage, and, in many cases, to restore urinary continence. The permanent indwelling catheter should remain excluded from the treatment of neurogenic lower urinary tract dysfunction. With adequate treatment, patients with neurogenic lower urinary tract dysfunction can be protected from severe complications and reintegrated into their normal social environment. After the acute phase of rehabilitation, urology is the most commonly required specialist area for paraplegic patients. In the past, urological problems have contributed most to the short lifespan of patients with an accident related spinal cord injury. Using modern neuro-urological treatment strategies, not only is lifespan increased but the quality of life of the patient is permanently improved.
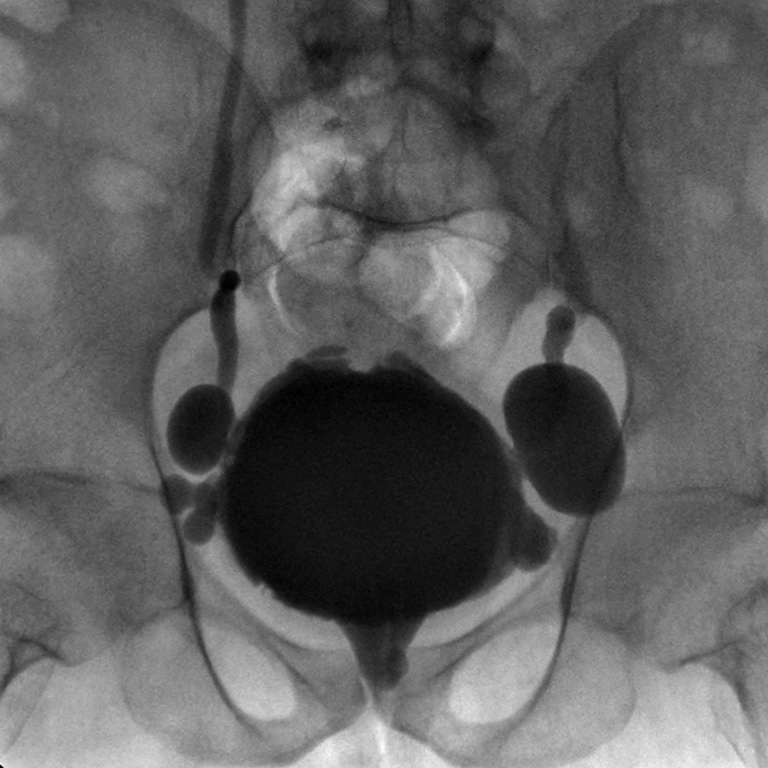
Legend
Nowadays, due to modern neuro-urological management, the typical neurogenic bladder with diverticula, pseudodiverticula, trabecula, and bilateral vesico-uretero-renal reflux damaging the upper urinary tract is rarely seen.
